
The new food pyramid gut health conversation has been heating up since the Dietary Guidelines for Americans (DGA) released their updated recommendations in January 2026.
Food guidelines often spark strong debate because they sit at the intersection of health, culture, identity, science, and lived experience.
The new upside-down pyramid is no exception.

What stands out most isn’t whether steak, butter, dairy, or eggs can fit into a healthy diet. It’s how unclear the model is about portion size, frequency, and context, especially when it comes to saturated fat and protein — two macro-nutrients that have a meaningful impact on gut health.
For women struggling with abdominal pain, bloating, gas, reflux, constipation, or diarrhea, these new food pyramid guidelines could directly influence gut inflammation, gut microbiome diversity, and potentially gut symptom flare-ups.
Feel less bloated, more energized, and in control of your digestion— in just 5 days.
A dietitian designed plan to calm your gut naturally.
Get Instant Access👇
Portion Size and Saturated Fat: What the New Food Pyramid Gut Health Model Misses
The pyramid visually emphasizes foods like steak, butter, beef tallow, and full-fat dairy and shows what appears to be a single serving as:
- A large cut of steak
- A whole chicken
- An entire stick of butter
- A full block of cheese
- A full carton of whole milk
At the same time, the written guidelines continue to recommend limiting saturated fat to no more than 10% of total daily calories.
This disconnect matters.
For a woman eating around 1,800 calories per day, that limit translates to roughly 20 grams / day of saturated fat total. That threshold can be reached easily:
- Ribeye, 3 oz → ~8 g
- 2 large eggs → ~3.5 g
- Butter, 1 tablespoon → ~7.3 g
- Hard Cheese, 1 oz → ~6 g
- Whole Milk Yogurt, ½ cup → ~2.5 g
That’s about 27.3 grams of saturated fat, already well over the recommended limit from foods many women eat in the same day (1). These foods can absolutely fit but large portions add up quickly and frequency matters.
When the visuals show abundance without context, it’s easy to assume “more is better,” even when the written guidance says otherwise.
I recently had a client message me (half joking, half serious):
“So… I can indulge in red meat and saturated fat now?”
The confusion is understandable.
Why Saturated Fat Matters for Gut Health
For women with gut sensitivities, oversized portions of saturated fats can exacerbate symptoms like bloating, gas, and intestinal inflammation. Understanding how the new food pyramid gut health model aligns—or doesn’t—with real-world portions is crucial.
Diets high in saturated fats have been shown to negatively alter gut microbiome composition, reduce microbial diversity, and promote pro-inflammatory bacterial profiles (like Fusobacteria). These can impair gut barrier function and trigger chronic digestive issues (2, 3, 4).
These effects are particularly relevant for individuals with a sensitive digestive system, as even moderate over-consumption may worsen symptoms and low-grade intestinal inflammation.
Understanding how portion sizes in the new food pyramid align—or don’t—with real-world consumption is therefore critical for practical dietary guidance.
Emphasizing small portions of saturated fats while prioritizing healthier unsaturated fats and fiber-rich foods can help support gut microbiome diversity and therefore quiet gut inflammation.
Unsaturated Fats: Where the New Food Pyramid Lacks Clarity for Gut Health but the Science Is Strong
Not all fats behave the same way in the gut. Unsaturated fats — particularly monounsaturated fats from olive oil and avocado oil, and omega-3-rich polyunsaturated fats from nuts, seeds, and fatty fish — consistently show benefits for gut microbiome health (5, 6, 7, 8).
These fats are associated with increased populations of short-chain fatty acid (SCFA)-producing bacteria, which help maintain the gut lining, reduce inflammation, and support immune balance (9).
For women with gut issues, this matters because SCFAs play a role in :
- Reducing gut pain and discomfort (common in IBS)
- Improving bowel regularity (relieves constipation or diarrhea)
- Calming bloating and fatigue
- Strengthening the gut lining to prevent leaky gut
- Supporting beneficial gut bacteria like Bifidobacterium and Faecalibacterium that produce SCFAs
- Regulating immune function by reducing pro-inflammatory cytokines
- Supporting metabolic health to improve insulin sensitivity and cholesterol levels (10, 11, 12)
Replacing some saturated fat with unsaturated fats has been shown to reduce pro-inflammatory microbial species and improve overall gut microbial balance.
By making unsaturated fats—like olive oil, fatty fish, avocado, nuts, and seeds—the primary source of fat in your diet you’re actively nurturing a diverse, resilient gut microbiome. You’ll reduce inflammation and create a digestive environment where beneficial bacteria can thrive.
For women struggling with bloating, bathroom irregularity, and gut discomfort, this simple shift can have a meaningful impact on long-term digestive health.
What About the Impact of Omega-6 Seed Oils on Gut Health?
This is where nuance is important.
Industrialized seed oils (soybean, corn, safflower) are a type of unsaturated fat that’s high in omega-6 fatty acids. In excess — especially when paired with ultra-processed foods — omega-6 intake may contribute to gut inflammation and microbial imbalance (13).
However, omega-6 fats from whole food sources like nuts, seeds, and plant foods behave very differently than refined, repeatedly heated oils found in processed foods (14).
For most women with gut symptoms, the most supportive approach is prioritizing:
- Using olive oil and avocado oil as their primary cooking fats
- Include nuts and seeds (chia, hemp, flax, walnuts) daily
- Eating fatty fish 1-2 times weekly
- Minimizing ultra-processed foods and industrialized seed oils
The new food pyramid gut health approach does emphasize healthy fats, but it’s important to know which ones truly support your microbiome.
For an 1,800-calorie day, subtracting ~20 g of saturated fat, from the example above, leaves roughly 24–50 g of unsaturated fats / day.
That looks like:
- 3 oz salmon → ~3.5 g
- ½ avocado → ~14.7 g
- 1 tbsp olive oil → ~14 g
- 1 tbsp chia seeds → ~3.4 g
- 10 walnut halves→ ~8.5 g
That equals 44.1g of healthy unsaturated fats for your day, well within the middle range of guidelines.
Making the right kind of unsaturated fats the main source of dietary fat supports long-term gut health and microbial diversity.
Protein Recommendations and Their Effect on Gut Health
Protein is often celebrated as a “must-have” for strength and vitality. However, when it comes to gut health, the amount, type, and context of protein intake can make a meaningful difference.
Too much protein, particularly from large portions of animal sources, can affect your gut microbiome and digestion in ways that aren’t immediately obvious.
While higher protein intake can support muscle mass, bone health, and functional capacity — particularly when paired with resistance training — protein needs aren’t static.
Protein is important but it isn’t one-size-fits-all.
Unlike the traditional Recommended Dietary Allowance (RDA), which was designed to prevent deficiency, the Acceptable Macronutrient Distribution Range (AMDR) was developed to reflect a wider range of protein intake. This change reflects the need to reduce risk of chronic disease, rather than a minimum threshold to simply avoid deficiency.
The AMDR guidelines provide a flexible range that accounts for individual variation in activity, age, and health status, making it a more practical guideline.
On an 1,800-calorie diet, the AMDR for protein suggests that an adult woman would benefit from approximately 45–158 grams of protein per day, which represents 10–35% of total daily calories. That’s quite a range!
The specific amount within this range will depend on factors such as activity level, life stage, overall health status, and more (27).
Protein Needs Vary Widely
Protein needs in a population can vary widely depending on:
- Physical activity level: Sedentary individuals require far less protein than someone doing strength training or endurance exercise
- Type of activity: Weightlifting and resistance training benefit from higher protein intake for muscle repair, while endurance exercise has different requirements
- Lean mass: needs will increase with more muscle mass
- Age: Older adults may need more protein to maintain muscle mass and support metabolic function
- Health status: Kidney disease, liver disease, or metabolic conditions can put limits on protein intake
- Life & Hormonal Stage: Pregnancy, lactation, perimenopause or menopause will affect needs
- Stress and recovery demands Recovery from surgery or injury increase protein requirements
- Daily fluctuations: Even in healthy adults, protein needs can vary day-to-day depending on activity, stress, and recovery demands, and more
This is why large, uniform portions of animal protein — like the oversized steak, whole chicken, or an entire carton of whole milk emphasized in the pyramid — aren’t generally appropriate. Most Americans aren’t sedentary, so their protein needs will typically be lower than what these visuals imply.
Here’s a handy reference for protein content per serving in both animal and plant sources:
- Sirloin (3 oz) → ~22.7 g
- Chicken Breast (3 oz) → ~26.3 g
- Salmon (3 oz) → ~21.6 g
- Shrimp (3 oz) → ~20.4 g
- 1 Hard boiled Egg → ~6g
- Greek yogurt (1/2 cup) → ~10.8 g
- Extra Firm Tofu (1/2 cup) → ~16.7 g
- Canned Chickpeas (1/2 cup) → ~5.8 g
- Lentils (1/4 cup) → ~6g
- Walnut halves (1/4 cup) → ~3.6 g
- Almond butter (1 tbsp) → ~3.2 g
- Hemp Seeds (1 tbsp) → ~2.5 g
source = Cronometer
Here’s a practical example:
- 2 eggs + + 3oz chicken breast + 3 oz salmon + 1/2 cup whole Greek yogurt + 1/4 cup hummus + 2 tbsp nut butter = 80 g protein, about 18% of calories on an 1,800-calorie diet.
Keeping protein portions in check can help support digestion, reduce gut inflammation, and maintain a healthy microbiome over time.
How High-Protein Diets Impact the Gut Microbiome
The updated pyramid increases protein recommendations by 50–100%, but not all women need high amounts of protein.
High-protein diets, particularly those heavy in animal protein and low in fiber, can negatively affect gut health in several ways. First off, they can increase your risk of developing Inflammatory Bowel Disease (IBD) (10, 11, 12).
When protein intake exceeds digestive capacity, excess protein reaches the colon, where it’s fermented by gut bacteria. This fermentation produces toxic metabolites such as ammonia, hydrogen sulfide, phenols, and indoles, which irritate the gut lining and increase inflammation and increase your risk for colorectal cancer (13, 14, 15).
Animal proteins, particularly red meat, can also increase bacteria that produce trimethylamine (TMA), which the liver converts to TMAO — a compound linked to systemic inflammation leading kidney and heart damage (16, 17).
Here’s an example of a stool test I use looking at protein breakdown and it’s inflammatory by-products produced in the gut (the first 4 rows):
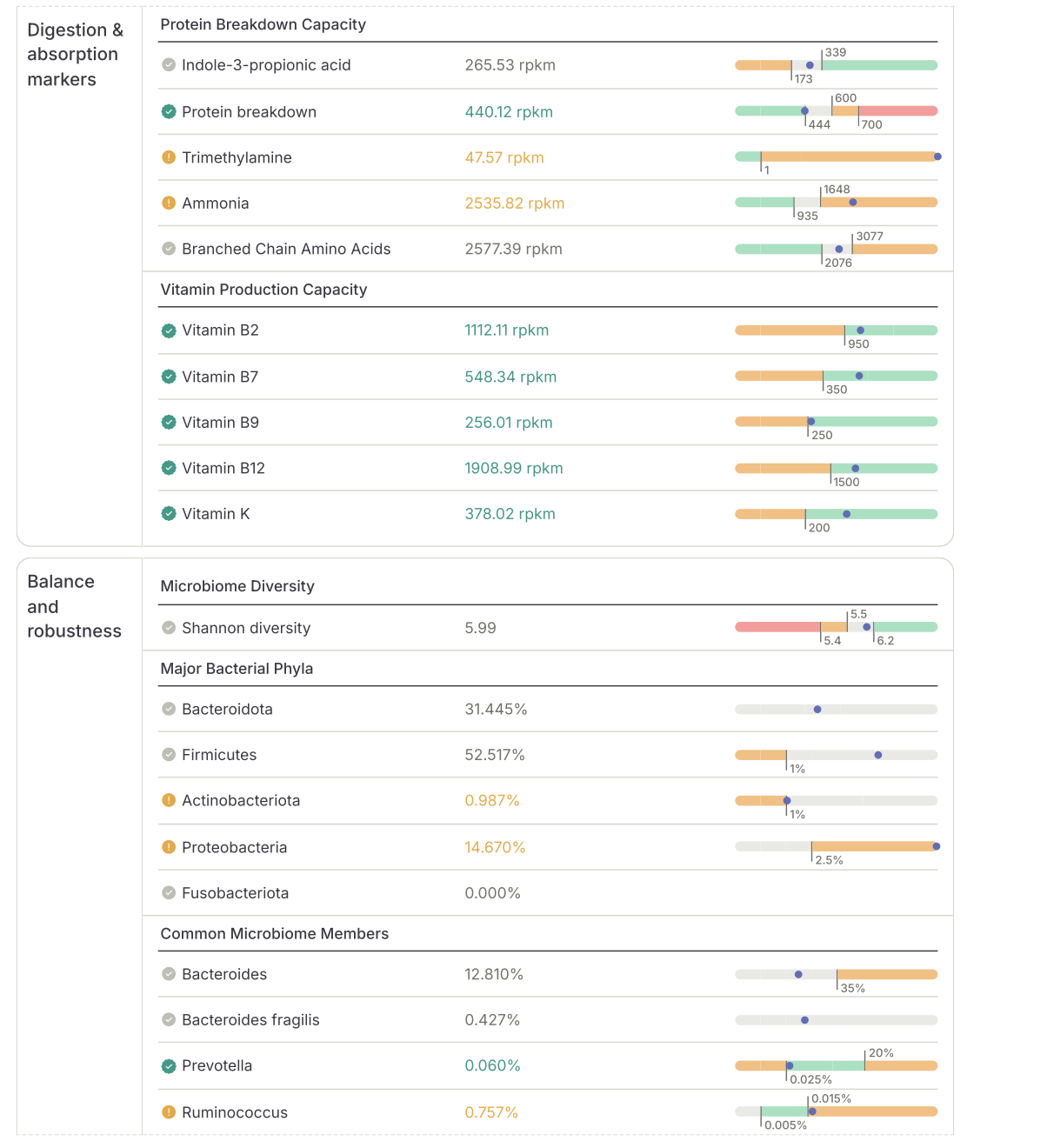
Diets high in red meat and saturated fat may further promote growth of bacteria like Methanogen and Bilophila, and Desulfovibrio species. These species increase gas production, slow gut transit (causing constipation), and contribute to overall gut inflammation (18, 19).
For women experiencing constipation, bloating, or gas, high animal protein intake often shows up as:
- A sensation of heaviness or sluggish digestion
- Increased gas and stronger, unpleasant odors
- Worsening constipation
- Reduced tolerance for high-protein foods
High-protein diets that are low in fiber reduce microbial diversity and slow gut transit, contributing to bloating, gas, and overall gut discomfort.
Protein quality matters. Animal proteins are more readily absorbed, but plant based proteins provide fiber, polyphenols, prebiotics, that feed beneficial gut bacteria and support SCFA production, helping reduce inflammation and promote digestive resilience (20, 21, 23, 24). Plant protein sources can include soy, legumes, beans, nuts, and seeds.
In practice, following the new food pyramid gut health recommendations means including a mix of plant and animal proteins in proper portions and always pairing animal protein with fiber (25).
Pairing animal proteins with fiber-rich vegetables, fruits, legumes, or whole grains helps maintain microbial balance and reduce pro-inflammatory metabolites (26).
Bottom Line: A mix of animal and plant proteins is ideal. For women with gut sensitivities, pairing protein with fiber-rich foods helps limit inflammatory metabolites, supports microbial diversity, and improves digestion. Large portions of animal protein, like the image of servings highlighted in the new food pyramid, may not be necessary or well-tolerated.
A Word on Protein Powders and the Gut Microbiome
Protein powders can be a convenient way to meet daily protein needs, but the type of protein and individual tolerances can influence gut health.
Animal protein powders, like collagen peptides, egg white, whey, casein, are highly bioavailable and efficiently absorbed, supporting muscle repair and bone health. However, for those with gut sensitivities, these powders can contribute to bloating, gas, or other digestive discomfort due to immune-mediated reactions or due to lactose intolerance (with whey particularly).
Plant protein powders, such as pea, soy, rice, or hemp, come with fiber, polyphenols, and prebiotics, which support beneficial gut bacteria and SCFA production as discussed above. They tend to ferment more slowly in the gut and may produce less TMAO-related inflammation. However, some individuals may still experience digestive issues depending on their unique microbiome composition or immune response to specific plant proteins.
Protein is a key nutrient particularly for women in perimenopause. While they experience a decline in estrogen, adequate protein is important to support muscle mass, bone health, hormone balance, and overall metabolic function.
Not all protein powders are created equal, however—how they are processed and their source (animal vs. plant) can influence gut microbiome composition and digestive tolerance. Always be careful of the additives (emulsifiers, flavorings, preservatives) used in these powders as they can also trigger gut issues too.
The chart below provides a snapshot of common protein powders, their protein content, and potential gut impacts to help guide informed choices.
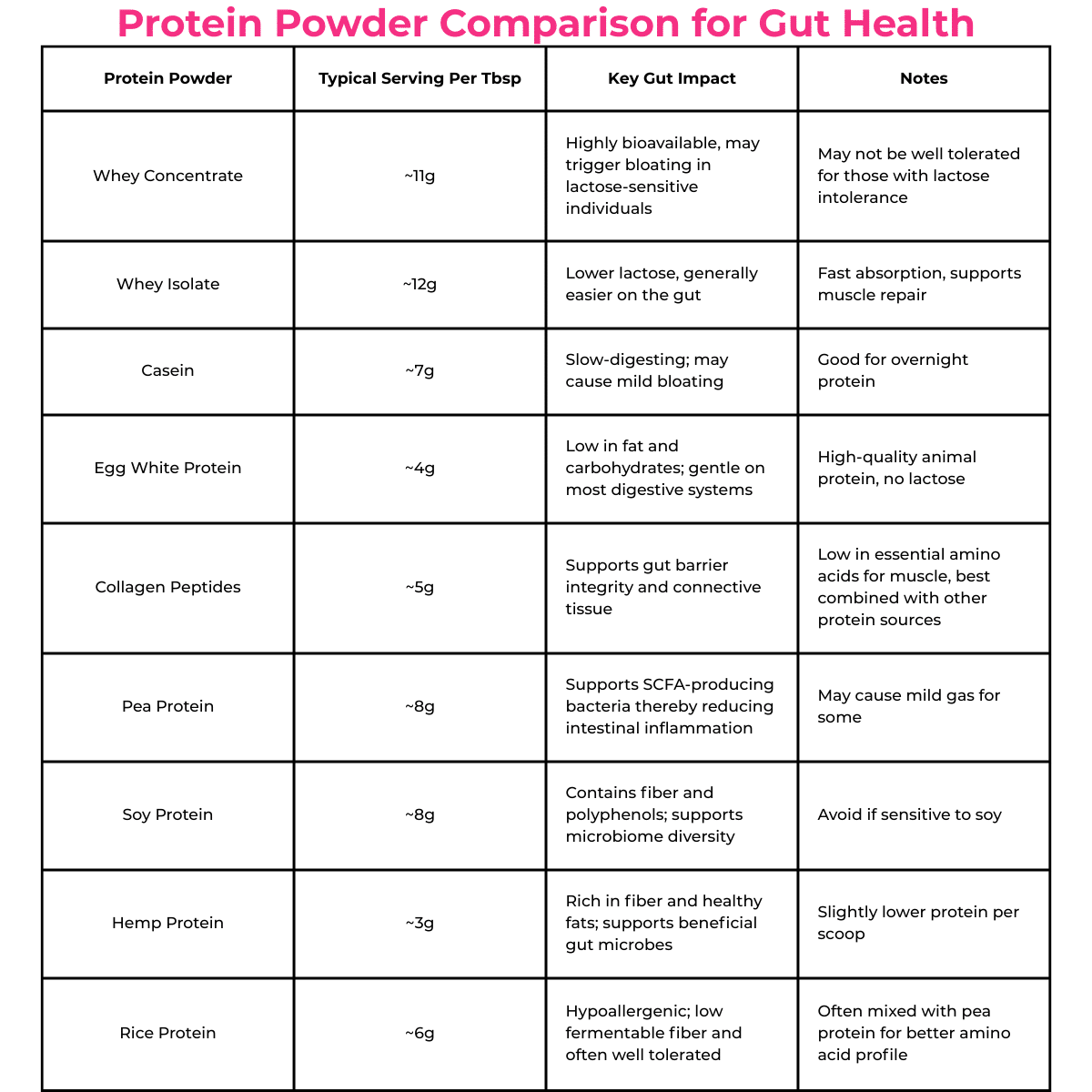
When choosing a protein powder, consider both your gut tolerance and nutritional needs. Pairing powders with fiber-rich foods, rotating between plant and animal sources can help minimize gut irritation and support microbiome diversity.
Protein powders like collagen peptides or egg white protein can complement whole foods, providing targeted benefits for digestion, connective tissue, and overall health for women, especially for those experiencing perimenopausal stomach problems.
The Summary About Selecting the Best Gut Friendly Protein Source
Even with carefully chosen protein sources, food sensitivities can play a key role in how the gut reacts. Food sensitivity testing, which measures Type III (immune complex-mediated) and Type IV (delayed T-cell-mediated) responses, can identify proteins that trigger low-grade inflammation or delayed digestive symptoms.

Type III reactions occur when antibodies form complexes with food antigens, potentially causing inflammation in the gut, while Type IV reactions involve T-cell activation and can produce delayed bloating, gas, or fatigue hours to days after eating.
For women, integrating food sensitivity test results can guide personalized protein choices, whether animal or plant-based. This approach helps support gut microbiome balance, reduces pro-inflammatory metabolites, and improves digestive comfort while still meeting protein goals.
Missing Gut-Healthy Foods in the New Food Guide Pyramid
While the updated food pyramid emphasizes fruits, vegetables, whole grains, and some healthy fats, it under-represents several key foods that support gut health that are especially important for women.
The brief mention on their website about the benefits of fermented foods on the microbiome is a great start, but more visibility in the imagery and guidance would better reflect current research on the microbiome.
Here’s a screenshot of their written guidelines:

When it comes to gut health, especially for women dealing with bloating, constipation, reflux, or irregular digestion, a few critical food groups are noticeably underrepresented and deserve a closer look:
- Legumes and beans: Lentils, chickpeas, black beans, and other legumes provide soluble fiber and prebiotics that feed beneficial gut bacteria.
- Polyphenol-rich foods: purple and red fruits and vegetables, walnuts, green tea, dark chocolate, and more act as “fertilizer” for a diverse microbiome.
- Fermented foods: While yogurt is highlighted, other fermented options like kefir, kimchi, sauerkraut, miso, and kombucha are equally important to introduce live beneficial microbes that strengthen the gut.
- Prebiotic-rich foods: Prebiotic foods that contain resistant starch—such as cooked then cooled rice or potatoes, green bananas, jicama and more—help selectively feed healthy gut bacteria.
- Spices and herbs: Turmeric, ginger, garlic, cinnamon, cloves, oregano, rosemary and more contain bioactive compounds that nourish and rebalance the microbiome, reduce gut inflammation, and aid digestion.
- Fiber variety: Women benefit from a broad array of fibers from nuts, seeds, and multiple colorful fruits, and vegetables to support gut health.
Research shows that adding a broader spectrum of fermented, prebiotic, and polyphenol-rich foods can ease bloating, constipation, diarrhea, and reflux by regulating motility and reducing gut inflammation.
What the New Food Pyramid Gut Health Model Gets Right
To be fair, the updated DGA does make meaningful improvements.
The shift away from ultra-processed foods and refined carbohydrates is a positive step. Emphasizing fruits, vegetables, and whole foods aligns strongly with what we know about gut health.
Higher fruit and vegetable intake supports microbial diversity, SCFA production, and improved stool regularity. Encouraging frozen produce also makes this more accessible and realistic.
Fiber remains central, with continued recommendations of about 14 grams per 1,000 calories, which is foundational for gut health.
In summary, the new food guide pyramid offers some positive shifts:
- Fruits and vegetables take center stage: Feeding SCFA-producing microbes and reducing inflammation.
- Shift away from processed carbs and packaged foods: Limiting refined breads, pastries, and sugary foods supports microbial diversity and stabilizes blood sugar.
- Fiber emphasis remains: The guideline still remains at ~14 g per 1,000 calories.
By prioritizing whole, fiber-rich plant foods, the guidelines support more consistent bowel movements and improved gut microbial balance. When implemented with appropriate portions and food variety, these changes can create a more stable digestive environment over time.
A More Digestive-Supportive Framework
The DGA’s are written for populations, not individuals. Gut health doesn’t improve by chasing macros or debating single nutrients in isolation. It improves through overall dietary patterns.
If you’ve been following the guidelines and still don’t feel well, the problem isn’t that you’re failing. It’s that the guidelines were never designed for individualized gut healing.
For women with digestive symptoms, meals are most supportive when they focus on:
- Whole, minimally processed foods
- A wide variety of colorful plants
- Mono and polyunsaturated fats as the primary fat source
- Moderate portions of animal protein paired with fiber
- Regular intake of legumes, fermented foods, polyphenol foods, and prebiotic foods
- Portions aligned with individual needs, labs, and symptoms
In Conclusion
The 2025–2030 DGAs make some meaningful improvements by emphasizing fruits, vegetables, and fiber but they still leave out other foods that truly support a healthy gut for women.
Legumes, fermented foods, prebiotic-rich starches, mono and polyunsaturated fats, polyphenol-packed foods, and gut-friendly spices and herbs aren’t highlighted enough, despite their critical role in supporting gut health.
At the same time, the highlighted oversized portions of saturated fat and animal protein could exacerbate abdominal pain, bloating, constipation, diarrhea, reflux, and other common digestive symptoms.
As a Registered Dietitian and Certified Microbiome Analyst, I help women go beyond generic guidelines. Using food sensitivity testing, comprehensive microbiome analysis, and micronutrient assessments, we uncover the true root causes to your gut issues.
Over a focused, 3 month Digestive Reset Program, we build a personalized plan that pairs the right proteins with fiber, incorporates fermented and prebiotic-rich foods, leverages polyphenols and spices, and emphasizes mono and polyunsaturated fats, all designed to restore microbial balance, reduce inflammation, and support long-term digestive comfort.
Gut health isn’t about following a one-size-fits-all pyramid or chasing perfection. It’s about understanding your unique needs, feeding your microbiome what it needs, and creating a sustainable, enjoyable way of eating that actually works.
With the right testing, guidance, and personalized support, women can finally feel vibrant, energized, and confident in their bodies—without guesswork, restriction, or repeated digestive setbacks.
Book your free call to get started on your gut healing program.
Feel less bloated, more energized, and in control of your digestion— in just 5 days.
A dietitian designed plan to calm your gut naturally.
Get Instant Access👇
With over 20 years of experience, Sarah Neumann Haske, MS, RDN, specializes in helping clients resolve chronic digestive issues through a root-cause approach. She holds a Master of Science in Human Nutrition, is a Certified Microbiome Analyst, and is the owner of Neumann Nutrition & Wellness, LLC. Through her 3-month gut healing program, clients can reduce reliance on medications, improve energy levels, and achieve sustainable, long-term healing.




