
Is Your Stomach Plotting Against You? Here’s What You Need to Know About Fructose Malabsorption
Let’s talk about that bloated, crampy, gas-filled, “why does my stomach hate me?” feeling that never seems to end. If that’s your reality, there’s a chance it could be Fructose Malabsorption throwing your gut for a loop, and not just the usual Irritable Bowel Syndrome (IBS) drama.
Fructose Malabsorption and IBS often share the same symptoms, which makes it tricky to figure out what’s really going on. But how can you tell which one is the real problem?
It’s simple, you can get yourself a hydrogen or methane breath test. It’s like a gut detective, zeroing in on the un-absorbed fructose causing chaos in your digestive system. Think of this test as the missing piece to the puzzle of your gut problems. As a bonus, I can help you interpret those results as part of my comprehensive 12 week Digestive Reset Program.
If you can’t do the breath test, you can still give your gut a break by cutting out fructose for a while and seeing if your symptoms ease up.
Fructose Intolerance Symptoms
Fructose intolerance, also called fructose malabsorption, occurs when your small intestine has difficulty absorbing fructose properly. This can lead to a range of uncomfortable digestive and systemic symptoms. Recognizing these signs can help you identify whether fructose might be contributing to your digestive issues.
Common Digestive Symptoms
- Bloating and gas – Unabsorbed fructose ferments in the gut, producing gas and causing bloating.
- Abdominal pain or cramping – Often felt in the lower or upper abdomen after eating fructose-rich foods.
- Diarrhea or loose stools – Fructose draws water into the intestine, leading to watery stools in some people.
- Constipation – In others, slow gut motility can occur due to the inflammatory process a food irritant is causing, leading constipation.
- Nausea or discomfort after meals – Especially after foods high in fructose or sorbitol.
Other Possible Symptoms
- Fatigue or brain fog – Some people notice low energy or difficulty concentrating after eating high-fructose foods.
- Headaches or migraines – Triggered by blood sugar fluctuations or gut stress.
- Joint or muscle discomfort – Possibly due to chronic inflammation from gut irritation in sensitive individuals.
Pattern to Look For
Symptoms typically appear 30 minutes to a few hours after eating fructose-containing foods. They can vary in severity depending on:
- The amount of fructose consumed
- Co-existing sugars (like sorbitol)
- Individual gut health and enzyme function
While these symptoms can overlap with IBS, lactose intolerance, or other digestive issues, a consistent reaction to fructose-containing foods is a strong clue that fructose malabsorption may be involved.
Feel less bloated, more energized, and in control of your digestion— in just 5 days.
A dietitian designed plan to calm your gut naturally.
Get Instant Access👇
What Foods Are Secretly Loaded With Fructose?
Fructose is hiding in more places than you’d think. It’s a monosaccharide (a fancy word for a simple sugar) and it comes in three forms in your diet: free fructose (found in fruits and honey), part of sucrose (aka regular sugar), and as fructans (a chain of fructose molecules) and in some veggies and wheat.
The biggest instigator? High Fructose Corn Syrup (HFCS)—and it’s in way more foods than you’d expect. Here’s a list to get you started:
- Soft drinks (they’re bad for you on so many levels)
- Ketchup & condiments (who would’ve thought!)
- Jams & jellies
- Yogurt & flavored milks (not as innocent as you think)
- Commercial breads (those store-bought loaves are sugar-loaded)
- Commercial salad dressings
- Cereals & breakfast foods (they’re basically sugar bombs)
- Crackers
- Maple syrup (unless it’s 100% pure, it’s got fructose in it)
So if you’re wondering why your stomach keeps acting up, take a closer look at your diet. Fructose is hiding in more foods than you might’ve thought.
How is Fructose Absorbed?
Your body can only handle so much fructose before it taps out. And right now we’re drowning in it. Fructose intake has tripled since the early 1900s—mostly thanks to all the added fructose in processed foods. Your gut has got a lot more to deal with than it ever did before.
When most people think of fructose, they think of fruit. Apples and oranges aren’t causing your troubles. A huge chunk of your daily fructose comes from foods you wouldn’t expect, like sodas, sauces, and snacks as mentioned above.
How exactly does your body break down fructose? For every fructose molecule that needs to be absorbed, it needs a glucose molecule. If that glucose isn’t around to pair up with it, that fructose just hangs out in your gut, causing problems.
That’s why sucrose (regular table sugar) tends to be easier to digest. It’s half glucose, half fructose, so your body has what it needs to handle it without issues.
Now, when it comes to fruit, some are easier on your stomach than others. Berries, citrus, and melons have more glucose than fructose, so they’re usually not a problem in smaller amounts.
And lastly, if you’re eating sugar alcohols—things like sorbitol, mannitol, or xylitol—you’re throwing a wrench into the works. These sugar substitutes mess with fructose absorption, and can leave your gut feeling like it’s been put through the wringer.
Your body has limits when it comes to fructose, and understanding how it all works (or doesn’t) is your ticket to a happier gut. Keep your eyes open to stop letting that excess fructose sneak up on you.
What Foods Should You Cut and What Should You Keep?
Alright, here’s how you tackle this whole fructose situation. First thing’s first: cut out the added fructose. That means anything with ingredients like fructose, crystalline fructose, HFCS (High Fructose Corn Syrup), corn syrup solids, agave, and honey needs to go. Yes, even honey—it’s not your gut’s BFF when it comes to fructose overload.
And don’t even think about those sugar-free products. They’re often loaded with sorbitol or xylitol, which will make things worse.
A fun fact: 1 can of soda has the same amount of fructose as 2 apples or 2 ounces of honey. So, if you’re thinking a soda’s no biggie, think again.
Also, keep an eye on medications or supplements that sneak fructose into their ingredient list. Not all fructose is obvious, and some of it might be hiding in places you wouldn’t expect.
Now, you might’ve heard that adding glucose (dextrose) to fructose-heavy foods can help your body absorb it better. Spoiler: research doesn’t back this up. Adding more sugar to sugar might seem like a quick fix, but it’ll probably just make things worse in the long run.
When it comes to fruits vs. veggies, fruits are the heavy hitters in the fructose department. A standard serving of fruit is 1/2 cup, and you’ll want to keep that to 2 servings a day max—but go for lower-fructose fruits. Think berries, citrus, and melons.
Veggies, on the other hand, are usually much easier on your gut. A serving is 1/2 cup, or 1 cup of leafy greens, and you can aim for 3-5 servings a day as tolerated.
Your gut’s the boss here. Listen to it, and keep your fructose intake in check.
A Quick List of High, Low and Zero Fructose Foods
Low Fructose Foods
Fruits
- Avocado
- Cranberries
- Lemon
- Lime
- Pineapple
- Oranges
- Kumquat
- Strawberries
- Bananas (no more than 1/3)
- Blueberries*
- Raspberries*
- Blackberries* (fresh and dried)
- Coconut*
- Clementine
- Kiwi
- Papaya
- Passion fruit
- Grapefruit
- Cantaloupe
- Honeydew
- Nectarines*
- Peaches*
- Plums*
Vegetables
- Bok choy*
- Carrots
- Celery*
- Chives
- Green pepper*
- Kale
- Parsnip
- Plum tomato
- Radish
- Rhubarb
- Spinach
- Lettuce
- Sweet potato*
- Turnip greens
- White potato
- Winter squash*
- Zucchini
- Olives
- Arugula
- Cucumber
- Green cabbage*
- Corn*
Cereals & Grains
- Wheat products with no HFCS (if tolerated)
- Corn products with no HFCS
- Crackers and pasta with no HFCS
- Grits
- Oatmeal
- Popcorn with no HFCS
- Quinoa
- Rice
Meats & Proteins
- Plain, unprocessed meats of any type
- Nut butters without HFCS
- Beans and legumes
- Tofu (can be gas forming)
Dairy & Substitutes
- Milk
- Cheese
- Yogurt
- Plant-based milks without HFCS
Sweeteners & Other
- 100% pure maple syrup
- White sugar
- Brown sugar
- Stevia
- Palm sugar
- Raw sugar
- Rice malt syrup
- Vanilla
- Dark chocolate
- Fats: olive oil, coconut oil, butter (if not lactose intolerant)
*Asterisk indicates high polyol or fructan content — consume in small amounts.

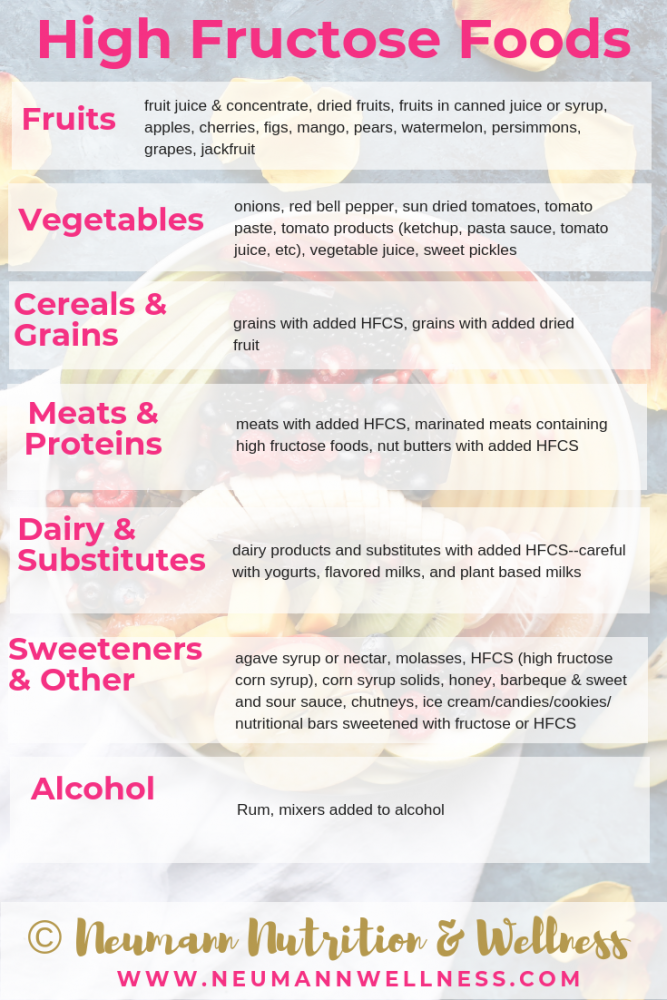
High Fructose Foods
Fruits
- Fruit juice and concentrates
- Dried fruits
- Fruits in canned juice or syrup
- Apples
- Cherries
- Figs
- Mangoes
- Pears
- Watermelon
- Persimmons
- Grapes
- Jackfruit
Vegetables
- Onions
- Red bell pepper
- Sun-dried tomatoes
- Tomato products (tomato paste, tomato sauce, salsa)
- V8 or other vegetable juice
- Sweet pickles
Cereals & Grains
- Grains with added HFCS or corn syrup solids
- Grains with added dried fruit
- Nutritional bars with added HFCS or dried fruit
Meats & Proteins
- Meats with added HFCS
- Marinated meats containing high-fructose foods
- Nut butters with added HFCS
Dairy & Substitutes
- Dairy and non-dairy products with added HFCS
Sweeteners & Other
- Agave
- Molasses
- HFCS (high fructose corn syrup) and corn syrup solids
- Honey
- Barbeque sauce
- Sweet and sour sauce
- Chutneys
- Ice cream, cookies, cakes, pies, candies sweetened with high-fructose sweeteners or HFCS
Alcohol
- Rum
- Mixers added to alcohol
Zero Fructose Foods
Here are some common foods that, per USDA, have 0 g of free fructose. These are useful when you’re trying to minimize fructose intake but still want nutrient-rich options.
Meats / Proteins
- Turkey, cooked, roasted (plain, no sauces)
- Pork, lean (unprocessed, unheated)
- Fish such as flounder, sole, cod, or other white fish
- Shrimp, plain
- Eggs
- Tofu (plain, unsweetened)
Vegetable Oils / Fats
- Olive oil
- Coconut oil
- Butter / Ghee (careful if you’re lactose intolerant)
Vegetables (Low Fructose + Low Sorbitol)
- Zucchini
- Lettuce and other leafy greens (spinach, kale, bok choy)
- Cucumber
- Radish
- Pumpkin
- Green beans
- Asparagus (in small portions)
- Carrot (in moderation)
Fruits (Low Fructose + Low Sorbitol)
- Citrus: Oranges, lemons, limes, tangerines (in moderate portions)
- Berries: Strawberries, blueberries, raspberries, blackberries (small servings)
- Melons: Cantaloupe, honeydew (moderate portions)
- Other: Papaya, kiwi, rhubarb
Tips for fruits:
- Stick to small to moderate portions, as even low-fructose fruits can trigger symptoms in larger amounts.
- Avoid apples, pears, mango, cherries, figs, watermelon, and plums, as they are high in fructose and/or sorbitol.
- Fresh or frozen fruits are usually better tolerated than dried fruits or juices, which concentrate sugars.
Grains / Starches
- Rice (white or brown, plain)
- Oats (plain)
- Plain pasta / noodles (no added sugar)
- Potatoes (white or sweet, in moderation)
Diary / Diary Alternatives
- Plain yogurt (unsweetened)
- Plain milk or lactose-free milk
- Hard cheeses (cheddar, Swiss, parmesan)
- Unsweetened plant-based milks (almond, oat, soy, without added sugar)
Other / Savory Items
- Plain nut butters (no added sugar or HFCS)
- Plain broths or stocks (no added sweeteners)
- Some strained vegetable purees (peas, carrots, squash) – check for additives
A Few More Tips Before You Go
Once you start your low-fructose diet, it’s important to stay on top of your progress. That’s where Practice Better comes in. As part of my 12-Week Digestive Reset Program, you’ll have access to this powerful tool to track your symptoms, meals, and any changes along the way. It’ll help you stay accountable and fine-tune your approach so your gut feels its best.
Still not sure about the fructose content of a specific food? No worries! You can easily check the USDA database by typing “fructose” and the food’s name into the search bar. Stick to foods that have less than 5g of fructose per serving to keep your gut on track: USDA Database
And remember, your tolerance to fructose depends on how much you’re eating at once. It’s also important to consider polyols and fructans if you’re still feeling off.
Feel less bloated, more energized, and in control of your digestion— in just 5 days.
A dietitian designed plan to calm your gut naturally.
Get Instant Access👇
Frequently Asked Questions (FAQs)
What vitamin deficiency causes fructose malabsorption?
Fructose malabsorption itself is not usually caused by a single vitamin deficiency, but certain nutrient deficiencies can impair the small intestine’s ability to absorb sugars, making symptoms worse.
From your post and research, the most important nutrients include:
- Zinc – Zinc is essential for maintaining a healthy brush border in the small intestine. The brush border contains microvilli that absorb sugars like fructose. Low zinc levels can impair enzyme function and microvilli repair, reducing fructose absorption.
- Vitamin B1 (Thiamine) and other B vitamins – These vitamins support carbohydrate metabolism. While not a direct cause, deficiencies may worsen sugar malabsorption symptoms by affecting how the body processes absorbed sugars.
- Vitamin A – Vitamin A helps maintain the integrity of the intestinal lining. Low vitamin A can contribute to intestinal inflammation and microvilli damage, which may reduce fructose absorption.
Bottom line: There isn’t a single “fructose malabsorption vitamin deficiency,” but deficiencies in zinc, vitamin A, and certain B vitamins can compromise gut health and the brush border, making fructose malabsorption more likely or severe. Supporting your gut with these nutrients can improve absorption and reduce symptoms over time.
Can fructose malabsorption be fixed?
Fructose malabsorption isn’t usually something that can be “cured” overnight, but it can be managed and often improved by understanding what triggers your symptoms and addressing the underlying causes.
Key points to consider:
- Identify your triggers – Not all fructose-containing foods affect everyone the same way. Keeping track of symptoms and testing foods systematically helps pinpoint at what dose and which specific fruits, vegetables, or processed foods are causing problems.
- Adjust your diet strategically – Rather than cutting out all fructose or all high-FODMAP foods permanently, you can use targeted adjustments to reduce symptoms while still nourishing your gut. For example, you might limit only certain high-fructose fruits or processed foods.
- Support digestion and gut health – Fructose malabsorption is often linked to impaired intestinal transport or dysbiosis. Improving gut health with the right nutrients, meal timing, and digestive support can help your body absorb fructose more efficiently over time.
- Avoid long-term strict restrictions – Overly restrictive diets can lead to nutrient deficiencies and even worsen gut health by starving beneficial bacteria. The goal is finding balance rather than total elimination.
Further information to consider is the health your intestinal brush border. Your brush border is the dense layer of microvilli lining the small intestine, and it plays a crucial role in digesting and absorbing nutrients, including sugars like fructose. When it’s damaged, nutrient absorption can be impaired, contributing to issues like fructose malabsorption or other digestive problems.
Here are the main reasons the brush border can become damaged:
1. Infections
- Bacterial, viral, or parasitic infections in the gut can inflame the small intestine and damage microvilli.
- Examples: Giardia, Rotavirus, Salmonella.
2. Chronic Inflammation
- Conditions like Celiac disease, Crohn’s disease, or autoimmune enteropathies trigger ongoing inflammation, which can erode the brush border.
- Even mild inflammation from food sensitivities or IBS-related immune activation may gradually reduce brush border function.
3. Poor Diet & Nutrient Deficiencies
- Diets lacking in zinc, vitamin A, or certain amino acids can impair microvilli repair.
- Overconsumption of processed foods, alcohol, or inflammatory fats can also harm the intestinal lining.
4. Toxins & Medications
- Certain medications like NSAIDs (ibuprofen, naproxen), chemotherapy drugs, or chronic antibiotics can irritate or damage the small intestine.
- Environmental toxins or chronic alcohol use can contribute too.
5. Gut Dysbiosis
- An imbalance of gut bacteria (too many harmful bacteria, too few beneficial bacteria) can trigger inflammation and produce toxins that damage microvilli.
- Overgrowth of bacteria in the small intestine (SIBO) is a common culprit.
6. Genetic or Structural Conditions
- Rare genetic disorders can impair brush border enzymes or microvilli formation, e.g., sucrase-isomaltase deficiency.
- Short bowel syndrome or surgery removing sections of the small intestine reduces brush border surface area
What foods are high in fructose?
When you’re dealing with IBS-like symptoms or suspect fructose malabsorption, it’s easy to assume the problem is just “fruit.” But as I explain in the post, fructose actually hides in far more places than you might expect—and that’s often why people stay stuck and confused.
Here are the main categories of high-fructose foods to pay attention to:
1. Foods with free fructose
These are foods where fructose isn’t paired with equal amounts of glucose, making it harder for your body to absorb.
Common examples include:
- Certain fruits like: fruit juice and concentrate, dried fruits, fruits in canned juice or syrup, apples, cherries, figs, mango, pears, watermelon, persimmons, grapes, jack fruit
- Certain vegetables like: onions, red bell pepper, sun dried tomatoes, tomato paste, tomato products (ketchup, salsa, tomato sauce), vegetable juice, sweet pickles
- Certain Grains like: any that have added HFCS (high fructose corn syrup), nutritional bars with added HFCS or high fructose sweeteners
- Certain Meats and Proteins like: any with added HFCS, marinated meats containing high fructose foods, nut butters with added HFCS
- Certain Dairy products like: any with added HFCS, flavored milks, non-dairy milks with added HFCS
- Certain Sweeteners or Sauces like: agave, molasses, HFCS, corn syrup solids, honey, barbeque sauce, sweet & sour sauce, chutneys
2. Processed foods with added fructose
This is where many people get tripped up because fructose is added to so many everyday products as HFCS (high fructose corn syrup) or corn syrup solids. You’ll often find it in:
- Sodas and sweetened beverages
- Ketchup and condiments
- Jams and jellies
- Sweetened yogurts and milk drinks
- Salad dressings
- Commercial breads
- Crackers
- Breakfast cereals
- Snacks
- Sweets like: Cakes, cookies, pies, candy
- Syrups (including many “maple” syrups that aren’t pure)
3. Fructans
These aren’t fructose themselves, but chains of fructose molecules. They’re found in foods like wheat products and certain vegetables, and they can trigger symptoms in a similar way if your body struggles to break them down.
4. Sugar alcohols (polyols)
While not technically fructose, sugar alcohols like sorbitol, mannitol, and xylitol can slow absorption and make fructose malabsorption symptoms worse—so they often sneak into the picture too.
With over 20 years of experience, Sarah Neumann Haske, MS, RDN, specializes in helping clients resolve chronic digestive issues through a root-cause approach. She holds a Master of Science in Human Nutrition, is a Certified Microbiome Analyst, and is the owner of Neumann Nutrition & Wellness, LLC. Through her 3-month gut healing program, clients can reduce reliance on medications, improve energy levels, and achieve sustainable, long-term healing.




